About This Article
This guide synthesizes peer-reviewed research and clinical guidelines from Johns Hopkins Medicine, the NHS, and the Endocrine Society. While the author is a health researcher, this content is for educational purposes only and not a substitute for professional medical advice.
Last Updated: February 2026 | Reading Time: 9 minutes
Have you ever felt like a stranger in your own body? Maybe your energy has vanished, your mood swings wildly, or your brain feels trapped in a permanent fog. Roughly 33% of men over 45 are living with clinically low testosterone (below 300 ng/dL), yet most don’t realize it until the symptoms become overwhelming.
Understanding the signs of low testosterone in men isn’t just about biology — it’s about reclaiming control of your health before exhaustion, weight gain, and mental fog take over. Whether you’re 35 or 65, recognizing testosterone deficiency early can be the first step toward feeling like yourself again.
In this article, you’ll discover:
- What testosterone actually does beyond building muscle
- The 5 warning signs most men overlook
- Science-backed lifestyle changes that boost testosterone naturally
- How to get tested and what your results really mean
The Bigger Picture: Testosterone’s True Role
While testosterone is famous for muscle mass and deep voices, its role extends far beyond the gym. It’s a metabolic engine that powers:
- Red blood cell production — Delivering oxygen throughout your body
- Bone density maintenance — Preventing osteoporosis and fractures
- Mood regulation — Influencing serotonin and dopamine pathways
- Cardiovascular health — Supporting healthy blood pressure and cholesterol
According to Johns Hopkins Medicine, testosterone isn’t just a “male hormone” — every human body produces and needs it to function optimally.
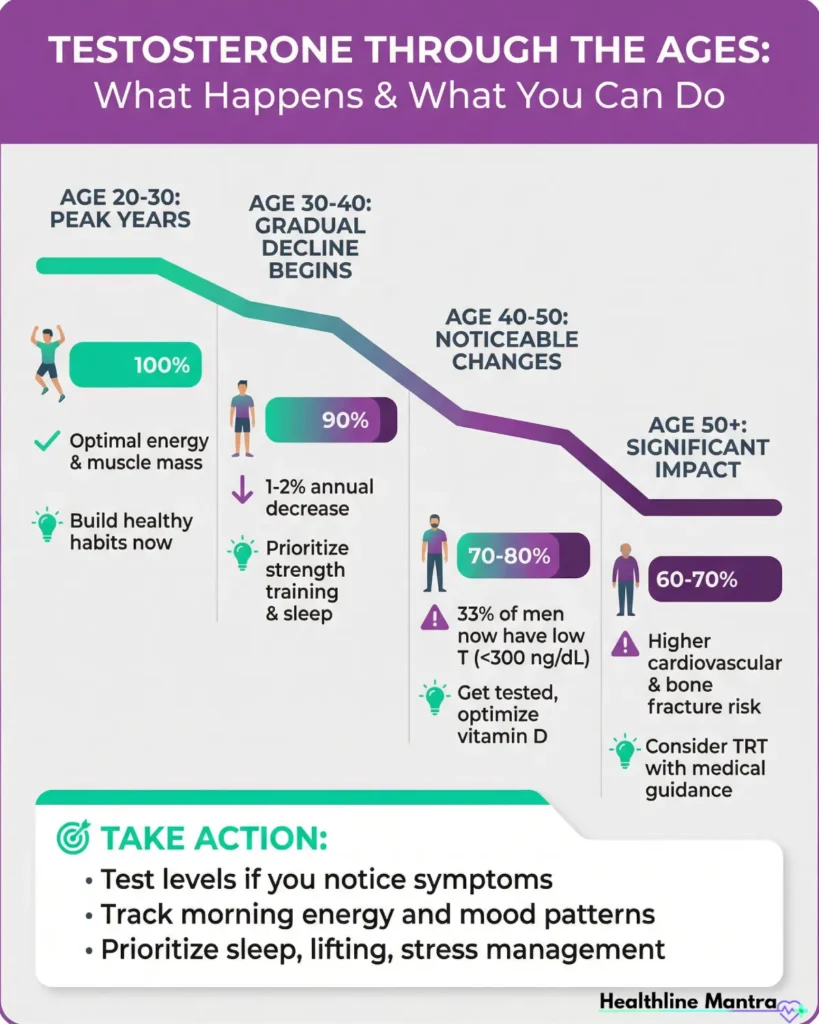
Here’s what’s concerning: Total testosterone naturally declines by about 1-2% each year after age 30. But modern lifestyle factors like chronic stress, poor sleep, and obesity are accelerating this decline, even in younger men.
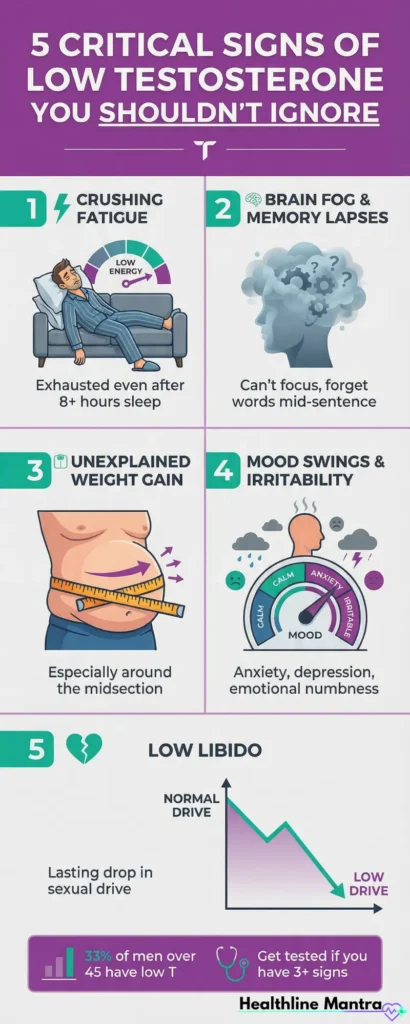
5 Critical Signs of Low Testosterone You Shouldn’t Ignore
The symptoms of testosterone deficiency often masquerade as “just getting older” or “work stress.” But when multiple signs appear together, it’s time to investigate further.
1. Crushing Fatigue That Sleep Doesn’t Fix
You’re getting 7-8 hours of sleep, yet you wake up exhausted. By mid-afternoon, you need willpower just to stay awake. This isn’t normal tiredness — it’s cellular-level energy depletion.
Why it happens: Testosterone plays a key role in mitochondrial function (your cells’ energy factories). When levels drop, so does your body’s ability to produce energy efficiently.
2. Brain Fog and Memory Lapses
You walk into a room and forget why. Words you’ve used your whole life suddenly escape you mid-sentence. Concentrating on tasks that used to be effortless now feels impossible.
Why it happens: Testosterone receptors exist throughout the brain, particularly in areas governing memory and cognitive function. Research shows low T is associated with reduced verbal memory and spatial abilities.
3. Unexplained Weight Gain (Especially Around the Midsection)
Despite eating the same and exercising regularly, belly fat keeps accumulating. You’ve tried cutting calories, but the weight won’t budge.
Why it happens: Low testosterone in men slows metabolism and increases fat storage, particularly visceral fat around the organs. Meanwhile, muscle mass — which burns calories at rest — decreases, creating a downward spiral.
4. Mood Volatility, Anxiety, or Depression
You’re irritable over small things. Anxiety creeps in without clear triggers. Or worse, you feel emotionally numb — disconnected from things that used to bring joy.
Why it happens: Men with low testosterone are nearly twice as likely to experience clinical depression. Testosterone influences neurotransmitter production, and declining levels disrupt emotional regulation.
5. A Noticeable, Lasting Drop in Libido
This isn’t about an occasional “not tonight” — it’s a complete disappearance of sexual desire that persists for weeks or months. Morning erections become rare or nonexistent.
Why it happens: Testosterone directly regulates sex drive and erectile function. When levels fall below 300 ng/dL, libido typically decreases significantly, often accompanied by erectile dysfunction.
The Health Risks You Can’t Ignore
Low testosterone in men isn’t just about feeling off — it carries serious long-term health consequences:
| Health Risk | Increased Danger |
| Cardiovascular mortality | 1.3x higher risk |
| Depression | 2x more likely |
| Bone fractures from osteoporosis | 2x higher risk |
| Metabolic syndrome | Significantly elevated risk |
According to the NHS, ignoring symptoms can lead to progressively worsening quality of life and increased disease burden.
What Causes Low Testosterone in Men?
Understanding the root causes helps you address the problem strategically:
Age-Related Decline
After age 30, testosterone drops 1-2% annually. By your 50s, cumulative loss can be substantial.
Obesity and Metabolic Issues
Excess body fat (especially belly fat) converts testosterone into estrogen through an enzyme called aromatase, creating a vicious cycle.
Chronic Stress
Persistent stress floods your system with cortisol, which directly suppresses testosterone production by 15%.
Sleep Deprivation
Most testosterone production happens during deep sleep. Consistently sleeping less than 7 hours can drop levels by up to 15%.
Medications
Opioid pain relievers, corticosteroids, and some antidepressants can significantly reduce testosterone.
Medical Conditions
- Type 2 diabetes
- Pituitary gland disorders
- Testicular injury or infection
- Hemochromatosis (excess iron)
- Sleep apnea
5 Science-Backed Ways to Boost Testosterone Naturally
Before considering medical intervention, these lifestyle changes can meaningfully improve testosterone levels:
1. Prioritize Strength Training
Compound lifts like squats, deadlifts, and bench presses trigger acute testosterone spikes of 15-20%. Aim for 3-4 sessions per week with progressive overload.
What the research shows: Studies demonstrate resistance training is among the most effective natural testosterone boosters, particularly when combined with adequate protein intake.
2. Protect Your Sleep
Testosterone production peaks during REM sleep. Men who sleep 4-5 hours have testosterone levels 10-15% lower than those sleeping 7-9 hours.
Action steps:
- Maintain consistent sleep/wake times
- Keep bedroom cool (65-68°F)
- Limit blue light exposure 2 hours before bed
- Consider sleep apnea screening if you snore heavily
3. Manage Blood Sugar and Insulin
High sugar intake spikes insulin, which signals the body to stop testosterone production. One study found that glucose consumption reduced testosterone by up to 25% for several hours.
Action steps:
- Minimize refined carbs and sugary drinks
- Prioritize protein and healthy fats
- Consider time-restricted eating (16:8 intermittent fasting)
4. Lower Chronic Stress and Cortisol
When cortisol rises, testosterone falls — it’s a biological trade-off. Chronic stress can suppress testosterone by 15% or more.
Action steps:
- Daily meditation or breathwork (even 10 minutes helps)
- Regular nature exposure
- Hobby engagement and social connection
- Professional therapy if stress feels unmanageable
5. Optimize Vitamin D Levels
Vitamin D acts almost like a hormone itself. Deficiency is closely linked to 20% lower testosterone levels. Research shows supplementation can increase levels, especially in deficient individuals.
Action steps:
- Get 10-30 minutes of midday sun exposure (depending on skin tone)
- Supplement with 2,000-4,000 IU daily if deficient
- Test levels annually — aim for 40-60 ng/mL
Foods That Support Healthy Testosterone
While no single food is a magic bullet, these nutrients matter:
| Food | Key Nutrient | Why It Helps |
| Oysters | Zinc | Critical for testosterone synthesis |
| Eggs | Cholesterol, Vitamin D | Testosterone is made from cholesterol |
| Fatty fish (salmon, mackerel) | Vitamin D, Omega-3s | Supports hormone production |
| Leafy greens | Magnesium | Involved in testosterone binding |
| Pomegranate | Antioxidants | May increase testosterone and improve blood flow |
| Brazil nuts | Selenium | Supports thyroid function (which affects testosterone) |
When to See a Doctor
You should get tested if you experience three or more of the following:
- Persistent fatigue despite adequate sleep
- Unexplained weight gain or difficulty losing fat
- Brain fog or memory issues
- Mood changes — irritability, anxiety, or depression
- Decreased sex drive or erectile dysfunction
- Loss of muscle mass or strength despite training
- Reduced body hair or facial hair growth
Important: These symptoms can also indicate thyroid disorders, depression, sleep apnea, or other conditions. A proper diagnosis is essential.
The Path Forward: Testing and Treatment
How Low Testosterone is Diagnosed
A simple blood test measures your testosterone levels. For accurate results:
- Test in the morning (7-10 AM) when levels peak
- Request both total and free testosterone — you need both for a complete picture
- Repeat the test if results are borderline (one low reading isn’t always diagnostic)
Understanding your numbers:
| Total Testosterone Level | Interpretation |
| Above 300 ng/dL | Generally normal (but “normal” varies by individual) |
| Between 200-300 ng/dL | Borderline; symptoms matter more than the number |
| Below 200 ng/dL | Clinically low; likely requires intervention |
According to the American Urological Association, diagnosis should be based on both lab results and symptoms, not numbers alone.
Treatment Options
Lifestyle Optimization (First-Line Approach)
Before considering medications, most doctors recommend 3-6 months of:
- Weight loss (if overweight)
- Resistance training
- Sleep improvement
- Stress management
- Addressing underlying conditions (diabetes, sleep apnea)
Many men see significant improvement from lifestyle changes alone.
Testosterone Replacement Therapy (TRT)
If lifestyle changes don’t help and levels remain low with persistent symptoms, TRT may be appropriate.
Common TRT methods:
| Method | Pros | Cons |
| Injections | Effective, inexpensive | Requires shots every 1-2 weeks; levels fluctuate |
| Topical gels | Steady levels, easy to use | Risk of transfer to others; daily application |
| Patches | Steady delivery | Skin irritation common |
| Pellets | Long-lasting (3-6 months) | Requires minor surgery; difficult to adjust dose |
Important considerations:
- TRT is lifelong — stopping can make you feel worse than before
- Can reduce fertility (sperm production decreases)
- Requires regular monitoring (blood work every 3-6 months)
- Not recommended if you want to have children soon
Cleveland Clinic emphasizes working with an experienced endocrinologist or urologist, not just a “hormone clinic.”
What Medical Experts Say
“Low testosterone in men is more than just a natural part of aging — it’s a treatable medical condition that significantly impacts quality of life,” explains Dr. Abraham Morgentaler, Associate Clinical Professor of Urology at Harvard Medical School, in his research on testosterone therapy.
According to the Endocrine Society’s clinical guidelines, men experiencing symptoms should be tested when levels are suspected to be below 300 ng/dL, particularly if experiencing “decreased libido, erectile dysfunction, reduced muscle mass, or persistent fatigue.” The American Urological Association further emphasizes that lifestyle modifications should be the first line of intervention before considering testosterone replacement therapy.
A Human-Centered Perspective
We’re living through an era of chronic stress, poor sleep, and sedentary lifestyles — and our bodies are struggling to keep up. If you suspect testosterone deficiency is affecting your quality of life, please listen to that instinct.
Your hormones are the silent architects of your physical and mental reality. When testosterone levels drop, even simple tasks feel overwhelming. But when you address the root cause — whether through lifestyle changes, medical treatment, or both — the fog lifts. Energy returns. Motivation resurfaces. You feel like yourself again.
You deserve to be the owner of your body, not just a passenger in it.
Key Takeaways
- Low testosterone affects 33% of men over 45 and increasingly impacts younger men
- Symptoms include fatigue, brain fog, weight gain, mood changes, and low libido
- Lifestyle changes — strength training, sleep, stress management, and nutrition — can significantly improve levels
- Get tested if you have 3+ symptoms; ask for both total and free testosterone
- TRT is an option but should be managed by a qualified specialist
If three or more of these signs sound familiar, book a morning testosterone blood test this week. It’s a simple draw that could change everything.
Disclaimer
This article provides general information for educational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or another qualified health provider with any questions you may have regarding low testosterone or other medical conditions.
Frequently Asked Questions
What are the most common symptoms of low testosterone in men?
The most common signs include persistent fatigue that sleep doesn’t fix, brain fog, unexplained weight gain around the midsection, mood swings or depression, and a noticeable drop in sex drive. Clinically low testosterone in men (below 300 ng/dL) also increases cardiovascular risk by 1.3x and doubles the risk of osteoporosis-related fractures.
At what age does testosterone start declining in men?
Testosterone naturally begins declining at roughly 1-2% per year after age 30. By age 45, approximately 33% of men have clinically low testosterone levels. However, lifestyle factors like chronic stress, poor sleep, obesity, and vitamin D deficiency can accelerate this decline at any age.
How can I increase my testosterone levels naturally?
Evidence-backed strategies include strength training (which can boost testosterone by 15-20%), sleeping 7-9 hours per night, reducing sugar intake to stabilize insulin, managing stress to lower cortisol, and correcting vitamin D deficiency. These lifestyle changes can meaningfully support healthy testosterone production without medication.
How is low testosterone diagnosed?
Low testosterone is diagnosed through a blood test, ideally performed in the morning (7-10 AM) when levels peak. The test should measure both total and free testosterone. Levels below 300 ng/dL are generally considered low, but optimal levels vary by individual, so discuss results with a knowledgeable healthcare provider.
Can low testosterone cause anxiety and depression?
Yes. Research shows men with low testosterone are nearly twice as likely to experience depression. Testosterone influences neurotransmitter function, and declining levels can cause irritability, anxiety, brain fog, and persistent low mood that’s often misdiagnosed as a standalone mental health condition.
What is the difference between total and free testosterone?
Total testosterone measures all testosterone in the blood, while free testosterone measures the small percentage (2-3%) not bound to proteins and actively available for the body to use. Both values are needed for an accurate diagnosis because a man can have normal total levels but low free testosterone.
Does low testosterone cause weight gain?
Yes. Low testosterone slows metabolism and increases fat storage, particularly visceral fat around the midsection. It also reduces muscle mass, which burns calories at rest, creating a cycle where weight gain becomes increasingly difficult to reverse through diet and exercise alone.
Is testosterone replacement therapy safe?
Testosterone replacement therapy (TRT) can be safe and effective when properly monitored by a qualified physician. However, it carries potential risks including reduced fertility, cardiovascular concerns (in some populations), and the need for lifelong treatment. It should only be used after lifestyle interventions have been tried and under close medical supervision.
Can stress lower testosterone?
Yes. Chronic stress elevates cortisol, a hormone that directly suppresses testosterone production by up to 15%. The relationship is inverse — when cortisol is high, testosterone tends to be low. Managing stress through meditation, exercise, adequate sleep, and social connection can help restore hormonal balance.
What foods help boost testosterone naturally?
Foods rich in zinc (oysters, beef), vitamin D (fatty fish, egg yolks), magnesium (leafy greens, nuts), and healthy fats (avocado, olive oil) support testosterone production. While no single food dramatically raises levels, a nutrient-dense diet combined with adequate protein and healthy fats creates the foundation for optimal hormone health.














